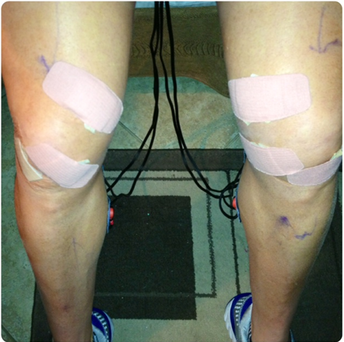
 In May of 2011, following the Buffalo Marathon, I injured my right knee. At the time, I had no idea what occurred. It was not until recently that I learned I have been running on a torn meniscus for 18 months. For the most part, I was able to overcome major issues by being proactive in managing my recovery. As an example, ice, stretching, rolling and myo-facial release helped alleviate a great deal of pain. In fact, between May of 2011 & August 2012, I trained for the Las Vegas Marathon & Ironman Louisville, raced regularly all with a torn meniscus and little to no problem associated with it. Only during large volume weeks did I experience pain and swelling with my injured knee. Two weeks ago while training for this year’s Las Vegas Marathon, I injured my left knee. My wife Lisa a Physician/Surgeon insisted this time that I see a Sports Physician about my injuries. Later, an MRI confirmed, bilateral medial meniscus tears. This was considered unusual as it generally would happen in one knee as opposed to both at the same time. Because the original injury took place in May of 2011, and my second injury a few weeks ago, it is easier to understand how these injuries occurred. I felt compelled to share this story and my road to recovery with my friends and the Triathlon community. This article will discuss and touch upon treatment options for such injuries and address how I opted to handle my own. As every athlete is different, what is best for me may not be best for you. I hope that this article will help shed light on this type of injury and the options athletes have when dealing with such injuries. My surgery was Friday December 14th, 2012. As I begin day 5 on new knees, I can feel my mobility coming back and the surgical pain subsiding much faster than I dreamed it would. I have not needed pain medication since day 2 and have decided to lower my dosage of Ibuprofen as well. I am still taking my daily aspirin to prevent DVT’s and clotting. Today will be my first day back on the bike. I plan to ride for 30-45 minutes in an easy spinning gear simply to start turning over the legs. This morning I added an abs wokout along with a few squats and lunges. The knees are starting to feel strong again and today I begin taking my first steps down the road to Wildflower. The remainder of this article is resource material on torn meniscus and treatment options for them. Please take some time to read this article if it interests you. Over the next few weeks, I will keep my blog up to date on my recovery and share with you my coach’s training plan. We plan to monitor the load closely over the next few weeks only adding as my knees can strengthen. I hope you will find this material both informational and educational…Stay tuned for updates on “As the Knees Return” over the next few weeks. Torn Meniscus Treatment There are many things to consider when deciding how to treat your torn meniscus, including the extent and location of the tear, your pain level, your age and activity level, your doctor's preference, and when the injury occurred. Your treatment choices are: Nonsurgical treatmentwith rest, ice, compression, elevation, and physical therapy. This may include wearing a temporary knee brace. Surgical repair to sew the tear together. Partial meniscectomy, which is surgery to remove the torn section. Total meniscectomy, which is surgery to remove the entire meniscus. This is generally avoided, because this option increases the risk for osteoarthritis in the knee. Whenever possible, meniscus surgery is done using arthroscopy, rather than through a large cut in the knee. This is how both of my knees were done. The location (zone) of the tear is one of the most important factors in determining treatment. See a picture of the meniscus zones. Tears at the outer edge of the meniscus (red zone) tend to heal well because there is good blood supply. Minor tears may heal on their own with a brace and a period of rest. If they do not heal or if repair is deemed necessary, the tear can be sewn together. This repair is usually successful in the red zone.· The inner two-thirds (white zone) of the meniscus does not have a good blood supply, so it does not heal well either on its own or after repair. If torn pieces float into the joint space, which may result in a "locked" knee or cause other symptoms, the torn portion is removed (partial meniscectomy) and the edges of the remaining meniscus are shaved to make the meniscus smooth. · When the tear extends from the red zone into the white zone, there may be enough blood supply for healing. The tear may be repaired or removed. This is something the orthopedic surgeon decides during the surgery. Also, the pattern of the tear may determine whether a tear can be repaired. Longitudinal tears are often repairable. Radial tears may be repairable depending on where they are located. Horizontal and flap (oblique) tears are generally not repairable. See a picture of different types of tears. Another factor when considering treatment is that repairs to the lateral meniscus (on the outer side of knee) typically heal better than repairs to the medial meniscus (on the inner side of the knee). See a picture of the lateral and medial menisci. It is preferable to preserve as much of the meniscus as possible. If the meniscus can be repaired successfully, saving the injured meniscus by doing a meniscal repair reduces the occurrence of knee joint degeneration compared with partial or total removal (meniscectomy). Meniscus repairis more successful in younger people (experts think people younger than about 40 years old do best), in knees that have good stability from the ligaments, if the tear is in the red zone, and if the repair is done within the first few weeks after the injury (acute).1 Meniscal repair may prevent degenerative changes in the knee joint. But it has not been proved conclusively that repairing a tear prevents more long-term problems (such as osteoarthritis) than not repairing a tear. Many doctors believe that a successful meniscus repair lowers the risk of early-onset arthritis because it reduces the stress put on the knee joint. Orthopedists most often perform meniscus surgery with arthroscopy, a procedure used both to examine and then to repair the inside of a joint by inserting a thin tube (arthroscope) containing a camera and a light through small incisions near the joint. Surgical instruments are inserted through other small incisions near the joint. Some tears require open knee surgery. Meniscus Tear: Should I Have Surgery? Rehabilitation varies depending on the injury, the type of surgery, your orthopedic surgeon's preference, and your age, health status, and activities. Time periods vary, but in general meniscus surgery is usually followed by a period of rest, walking, and selected exercises. After you have full range of motion without pain and your knee strength is back to normal, you can return to your previous activity level. For some exercises you can do at home (with your doctor's approval), see: Meniscus Tear: Rehabilitation Exercises. My road to recovery is coming along faster than I had imagined. The post surgical pain associated with this procedure is minimal. I can already tell that I am getting stronger and the acute pain I once experienced in my knees is gone. As I slowly return to fitness, I will keep you all informed as to how things progress. 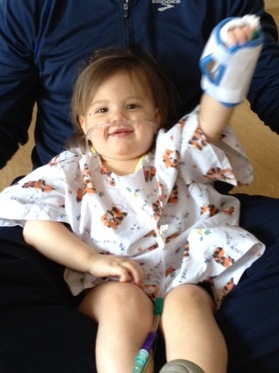 RSV (Respiratory Syncytial Virus)--Report Many of you are expecting to see this year’s Las Vegas Marathon & ½ Marathon Race Report. The race begins later today and unfortunately this year Lisa and I were unable to attend. On Wednesday last week, we took Eva to see our pediatrician and he in turn sent us immediately to the ER at Children’s Memorial Hospital. Eva was under severe respiratory distress and her Oxygen saturation was reading in the middle to low 80’s. We learned later that Eva had gotten a virus called RSV (Respiratory Syncytial Virus). This is a nasty little bug. Lisa and I thought we should write about RSV as a means to help educate parents on RSV, how to prevent it, and how to recognize the early signs in order to keep your loved ones from being hospitalized due to RSV. Respiratory syncytial (sin-SISH-uhl) virus, or RSV, is a respiratory virus that infects the lungs and breathing passages. Most otherwise healthy people recover from RSV infection in 1 to 2 weeks. however, infection can be severe in some people, such as certain infants, young children, and older adults. In fact, RSV is the most common cause of bronchiolitis (inflammation of the small airways in the lung) and pneumonia in children under 1 year of age in the United States. In addition, RSV is more often being recognized as an important cause of respiratory illness in older adults. RSV can cause upper respiratory infections (such as colds) and lower respiratory tract infections (such as bronchiolitis and pneumonia). In children under 1 year of age, RSV is the most important cause of bronchiolitis, an inflammation of the small airways in the lung. Almost all children will have had an RSV infection by their second birthday according to the CDC. When infants and children are exposed to RSV for the first time, 25% to 40% of them have signs or symptoms of bronchiolitis or pneumonia, and 0.5% to 2% will require hospitalization. Most children hospitalized for RSV infection are under 6 months of age. Infants and children infected with RSV usually show symptoms within 4 to 6 days of infection. Most will recover in 1 to 2 weeks. However, even after recovery, very young infants and children with weakened immune systems can continue to spread the virus for 1 to 3 weeks. People of any age can get another RSV infection, but later infections are generally less severe. The elderly and adults with chronic heart or lung disease or with immune systems weakened by medical conditions or treatments remain at high risk for developing severe RSV disease if reinfected. In temperate climates, RSV infections generally occur during fall, winter, and early spring. The timing and severity of RSV circulation in a given community can vary from year to year. How is RSV spread? RSV can be spread when an infected person coughs or sneezes into the air. Coughing and sneezing send virus-containing droplets into the air, where they can infect a person if they inhale these droplets or these droplets come in contact with their mouth, nose, or eye. Infection can also result from direct and indirect contact with nasal or oral secretions from infected persons. Direct contact with the virus can occur, for example, by kissing the face of a child with RSV. Indirect contact can occur if the virus gets on an environmental surface, such as a doorknob, that is then touched by other people. How can RSV infection be prevented? Researchers are working to develop RSV vaccines, but none is available yet. However, there are steps that can be taken to help prevent the spread of RSV. Specifically, people who have cold-like symptoms should cover their coughs and sneezes. Wash their hands frequently and correctly (with soap and water for 15–20 seconds) Avoid sharing their cups and eating utensils with others. Refrain from kissing others. In addition, cleaning contaminated surfaces (such as doorknobs) may help stop the spread of RSV. Special attention should be paid to protecting children who are at high risk for developing severe disease if infected with RSV. Such children include premature infants, children under 2 with chronic lung or heart conditions, and children with weakened immune systems. Ideally, people with cold-like symptoms should not interact with children at high risk for severe disease. But, if this is not possible, they should carefully follow the prevention steps mentioned above, and they should wash their hands before interacting with children at high risk. When possible, limiting the time that high-risk children spend in child-care centers or other potentially contagious settings may also help prevent infection and spread of the virus during the RSV season. Helpful Hints to help Prevent RSV A drug called palivizumab (say "pah-lih-VIH-zu-mahb") is available to prevent severe RSV illness in certain infants and children who are at high risk. The drug can help prevent development of serious RSV disease, but it cannot help cure or treat children already suffering from serious RSV disease and it cannot prevent infection with RSV. If your child is at high risk for severe RSV disease, talk to your healthcare provider to see if palivizumab can be used as a preventive measure. Lisa and I, pulled the majority of this information from the Center for Disease Controls website. If you have any questions about RSV please contact your medical provider. We hope this helps you and your family becomes familiar with the warning signs of RSV. |
 RSS Feed
RSS Feed